| World Journal of Nephrology and Urology, ISSN 1927-1239 print, 1927-1247 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, World J Nephrol Urol and Elmer Press Inc |
| Journal website http://www.wjnu.org |
Case Report
Volume 6, Number 3-4, October 2017, pages 32-34
Salmonella typhi Bacteriuria, Predispositions and Complications: Two Case Reports and Review of Literature
Reetika Dawara, d, Sanjiv Jasujab, Firdaus Imdadia, Nitin P. Ghongec
aDepartment of Microbiology, Indraprastha Apollo Hospitals, Sarita Vihar, New Delhi, India
bDepartment of Nephrology, Indraprastha Apollo Hospitals, Sarita Vihar, New Delhi, India
cDepartment of Radiology, Indraprastha Apollo Hospitals, Sarita Vihar, New Delhi, India
dCorresponding Author: Department of Microbiology, Indraprastha Apollo Hospitals, Sarita Vihar, New Delhi 110076, India
Manuscript submitted May 24, 2017, accepted June 9, 2017
Short title: Salmonella UTI
doi: https://doi.org/10.14740/wjnu310w
This article has been retracted
| Abstract | ▴Top |
Salmonella typhi infection presents most commonly as typhoid fever and infrequently as extraintestinal localized infections of bone, joints, soft tissues, spleen, endocarditis, pulmonary, hepatobiliary, genital and urinary systems. Urinary tract infection (UTI) is rare and clinical presentation is indistinguishable from UTIs due to other etiological agents or may even be asymptomatic. We report two cases of patients with chronic kidney disease with UTI due to Salmonella typhi. Renal cyst, nephrolithiasis and urethral strictures were the concomitant findings in one case and renal tubular acidosis with nephrocalcinosis in the other. In patients with relapses and a chronic course with coexisting functional or structural abnormalities of the urinary tract system, the suspicion of salmonella as one of the probable causative agents should be kept in mind so as to ensure appropriate and adequate therapy. Also in the presence of long-standing hypokalemia, one must investigate for renal abnormalities and vice versa.
Keywords: Chronic kidney disease; Nephrocalcinosis; Nephrolithiasis; Salmonella; Urinary tract infection
| Introduction | ▴Top |
Salmonellosis may manifest as gastroenteritis, enteric fever, localized infection, or carrier state. One million foodborne illnesses in USA are due to salmonella infection [1]. Enteric fever is endemic in many tropical countries.
Predisposing conditions like hemoglobinopathies, joint trauma, surgery, cholelithiasis or other immunosuppressive states have been documented in patients with extraintestinal manifestations [2]. We present here two cases of UTI due to Salmonella typhi and their associated predisposing conditions from our hospital in North India.
| Case Reports | ▴Top |
Case 1
A 56-year-old male patient presented to Indraprastha Apollo Hospitals, New Delhi with complaint of off and on right flank pain for the last 1 month. He was admitted for further evaluation and management. Abdomen ultrasound (USG) and contrast-enhanced computed tomography findings were suggestive of large pelviureteric junction calculus with marked back pressure and left upper pole calculus. 99m Tc DTPA Renal Dynamic Study showed subnormal glomerular filtration rate (GFR), left side non-obstructed kidney and right enlarged partially obstructed kidney with moderately impaired cortical function.
Right DJ stenting was done (Fig. 1). His urine routine microscopy (R/M) showed raised proteins and pus cells full high power field. Patient was started empirically on ofloxacin 200 mg orally 12 hourly. Urine culture showed pure growth of > 100,000 CFU/mL of urine of non-lactose fermenting colonies on MacConkey Agar. These were identified as Salmonella typhi on Vitek 2 Compact and Vitek MS (Biomerieux, France). Agglutination with salmonella polyvalent O antisera (Denka Seiken, Japan) and salmonella O antiserum factor 9 (Becton Dickinson and Company, Ltd) were positive.
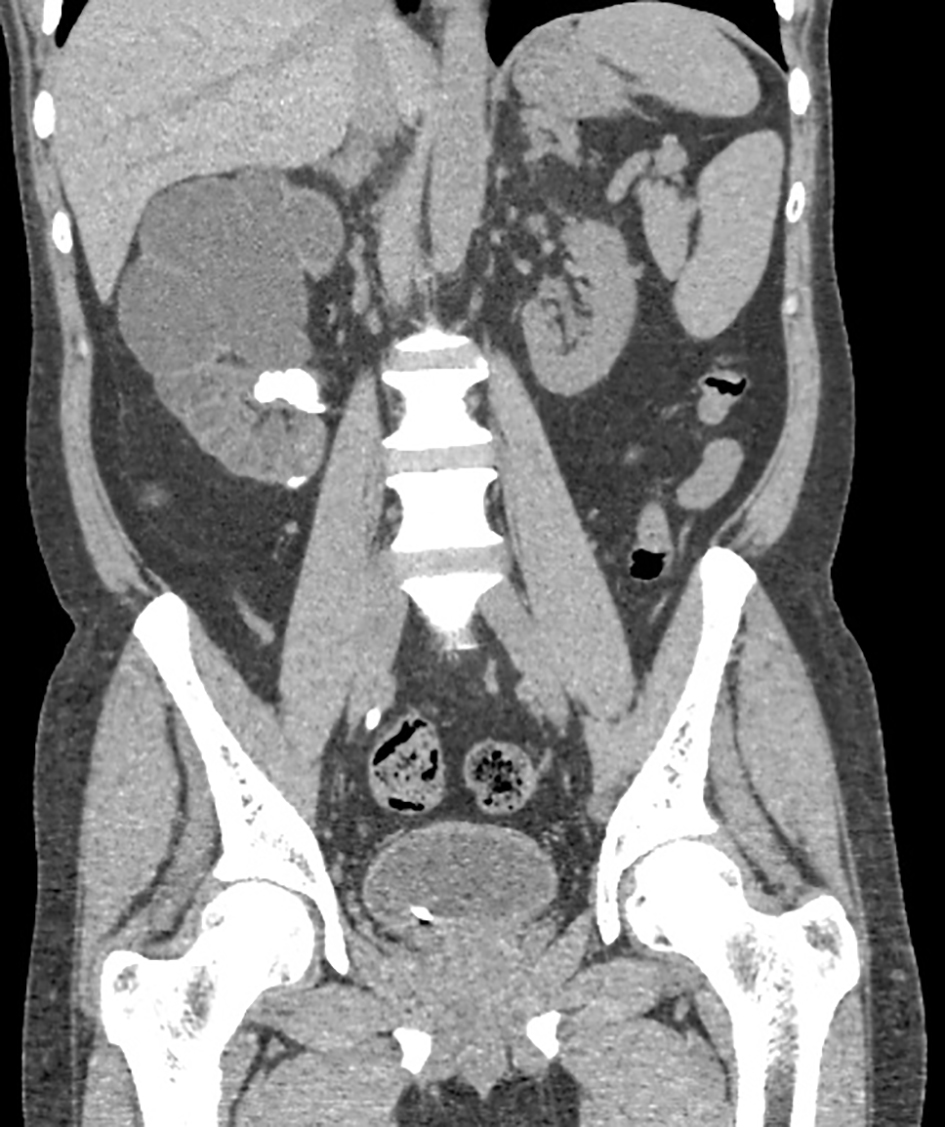 Click for large image | Figure 1. Coronal NCCT image showing gross hydronephrosis involving the right kidney with calculus in the lower major calyx and gross parenchymal thinning. Ureteric stent is also noted on the right side. |
Antibiotic susceptibility testing done and interpreted following CLSI guidelines [3] showed strain was sensitive to ceftriaxone and cefexime and resistant to ampicillin, nalidixic acid, cotrimoxazole and quinolones. Following the sensitivity report, antibiotic treatment was changed to cefixime 200 mg twice a day for 2 weeks and patient was advised to come for follow-up and evaluation of renal functions. Percutaneous nephrolithotomy (PCNL) was planned if the renal functions improved. On follow-up after 2 weeks, his serum urea level was 75 mg/dL (reference range 10 - 50 mg/dL), serum creatinine was 2.4 mg/dL (reference range 0.5 - 1.3 mg/dL) and urine R/M still showed pus cells full field. Abdomen USG showed right-sided hydronephrosis with renal calculus and left renal cyst. The same antibiotics were continued and his renal parameters were monitored. After 6 weeks, PCNL was performed and urine, stones and DJ cultures were sent to the microbiology laboratory. All the three revealed growth of Salmonella typhi with the same antibiotic susceptibility pattern as earlier. Thus, the treatment was continued for another 2 weeks.
DJ stent was removed after 2 months. At this time, the urine culture showed no growth of Salmonella typhi. After 2 years, patient presented with pain and swelling of left side of scrotum.
Uroflowmetry was suggestive of obstructive pattern. Retrograde urethrogram and micturating cysto-urethrogram were suggestive of proximal penile urethra stricture. Cystoscopy and optical internal urethrotomy were performed. S. creatinine started improving and patient was discharged in a stable condition.
Case 2
A 27-year-old male patient presented for evaluation of weakness since last month and complaints of difficulty in walking. Over the last 4 years, he had been hospitalized four times with episode of extreme muscle weakness in his hometown and received I/V therapy for low potassium levels. His past history revealed inability to hear and speak since 4 months of age and persistent hypokalemia since childhood. Patient was thoroughly evaluated and found to have distal renal tubular acidosis with nephrocalcinosis on abdomen USG. Investigations ruled out sickle cell anemia, hypercalciuria, hyperglobulinemia and cirrhosis.
Potassium levels were optimized with oral potassium citrate solution. Urine culture revealed Salmonella typhi colony count > 105/mL and the isolate was sensitive to amoxicillin and clavulanate, cefotaxime, ceftriaxone, cotrimoxazole, nalidixic acid and quinolones. Patient was started on cefexime 200 mg daily till next follow-up after 2 weeks. He was discharged in stable condition.
| Discussion | ▴Top |
Salmonella enters the urinary tract either hematogenously following a recent episode of typhoid fever once a threshold of the organism is reached in the bloodstream or in chronic carrier states involving the urinary system or by direct invasion of the bladder via the urethra through fecal contamination [4].
The two cases reported by us represent true UTIs, as opposed to colonization or fecal contamination, by virtue of being isolated in pure culture and in high concentrations (> 100,000 CFU/mL).
Salmonella was reported as the cause of 0.056-0.07% of UTIs in Spain and 0.002-0.0037% of UTIs in the United States [5]. Although S. typhi bacteriuria is rare even where it is endemic, this specific infection should be kept in mind in patients who have an unidentified chronic UTI.
Interstitial nephritis and renal micro-abscesses can develop as important complications in the course of salmonella UTI. Salmonella emphysematous pyelonephritis has been reported in a non-diabetic and non-obstructive end-stage renal disease patient from Taiwan [6].
Recent surveys of salmonella bacteriuria have focused on risk factors associated with acquisition of UTIs. Such risk factors include immunocompromised conditions, underlying urologic abnormalities, neoplasms of the kidney, nephrolithiasis, hydronephrosis, anatomic abnormalities, schistosomiasis, tuberculosis, prostatic hypertrophy, renal transplant recipients, and lupus nephritis [7, 8]. Many of these cases do not have a past history of typhoid fever [8]. In our patients, no past history of typhoid fever was documented.
Many cases of bacteriuria do occur in individuals without known risk factors. An Australian investigation by Paterson and colleagues of 23 persons with Salmonella UTIs (> 1,000 leukocytes/mL, > 105 CFU/mL) identified no immunocompromised patients in their study and only three (13%) with urologic abnormalities [9].
In our second case, there was history of treatment with Kanamycin in childhood which is known causes of deafness and renal damage. Hypokalemia results in addition to an alkaline urine and bladder dysfunction leads to urinary stasis and luxuriant bacterial growth.
Antibiotic treatment is challenging and prolonged treatment is indicated due to chronic bacteriuria and relapses [9]. Thus, it is crucial to request for repeat urine cultures in follow-ups. In case of a UTI associated with anatomic obstructive abnormalities, surgical correction may be required in addition to prolonged antimicrobial therapy (≥ 6 weeks) to eradicate infection [10].
Prolonged course of antibiotic treatment with cephalosporins, surgical removal of the calculi and drainage procedure in conjunction helped in cure in our cases.
Conflict of Interest
None.
Funding Source
None.
| References | ▴Top |
- http://www.cdc.gov/foodborneburden Jan 2012.
- Mathuram A, Rijn RV, Varghese GM. Salmonella typhi rib osteomyelitis with abscess mimicking a 'cold abscess'. J Glob Infect Dis. 2013;5(2):80-81.
doi pubmed - CLSI. Performance standards for Antimicrobial Susceptibility testing, 26th edition, CLSI supplement M100S. Wayne PA: Clinical and Laboratory Standards Institute, 2016.
- Huang DB, DuPont HL. Problem pathogens: extra-intestinal complications of Salmonella enterica serotype Typhi infection. Lancet Infect Dis. 2005;5(6):341-348.
doi - Tena D, Gonzalez-Praetorius A, Bisquert J. Urinary tract infection due to non-typhoidal Salmonella: report of 19 cases. J Infect. 2007;54(3):245-249.
doi pubmed - Tsai JP, Fang TC, Wang CH, Hsu BG. Case report - salmonella emphysematous pyelonephritis in a nondiabetic and non-obstructive end - stage renal disease patient. Tzu Chi Med J. 2007;19(4).
- Ramos JM, Aguado JM, Garcia-Corbeira P, Ales JM, Soriano F. Clinical spectrum of urinary tract infections due to nontyphoidal Salmonella species. Clin Infect Dis. 1996;23:388-390.
doi pubmed - Mathai E, John TJ, Rani M, Mathai D, Chacko N, Nath V, Cherian AM. Significance of Salmonella typhi bacteriuria. J Clin Microbiol. 1995;33(7):1791-1792.
pubmed - Paterson DL, Harrison MW, Robson JM. Clinical spectrum of urinary tract infections due to nontyphoidal Salmonella species. Clin Infect Dis. 1997;25(3):754.
doi pubmed - Cohen PG. The pathogenesis of recurrent urinary tract infection: the bowel, bladder hypokalemia connection. Med Hypotheses. 1983;10(1):1-4.
doi
This article is distributed under the terms of the Creative Commons Attribution Non-Commercial 4.0 International License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
World Journal of Nephrology and Urology is published by Elmer Press Inc.
